Key Takeaway (2026 Summary)
What are the E/M coding changes for 2026?
Effective January 1, 2026, the E/M coding guidelines continue to emphasize Medical Decision Making (MDM) and minimum time thresholds. Additionally, new updates highlight AI-assisted coding, cognitive work recognition, and expanded remote monitoring services (99453–99454). As a result, coders must now evaluate not only documentation complexity but also how technology and clinical judgment contribute to code selection.
Introduction: Why the 2026 E/M Update Matters
As we move into 2026, Evaluation and Management (E/M) coding continues to evolve toward accuracy, efficiency, and real-world clinical relevance. Previously, the shift away from history and exam scoring changed how coders approached documentation. Now, however, the focus goes even deeper.
Specifically, the 2026 updates emphasize cognitive labor, AI-assisted data review, and digital health integration. Therefore, coders must not only understand traditional MDM—but also how modern tools influence provider decision-making.
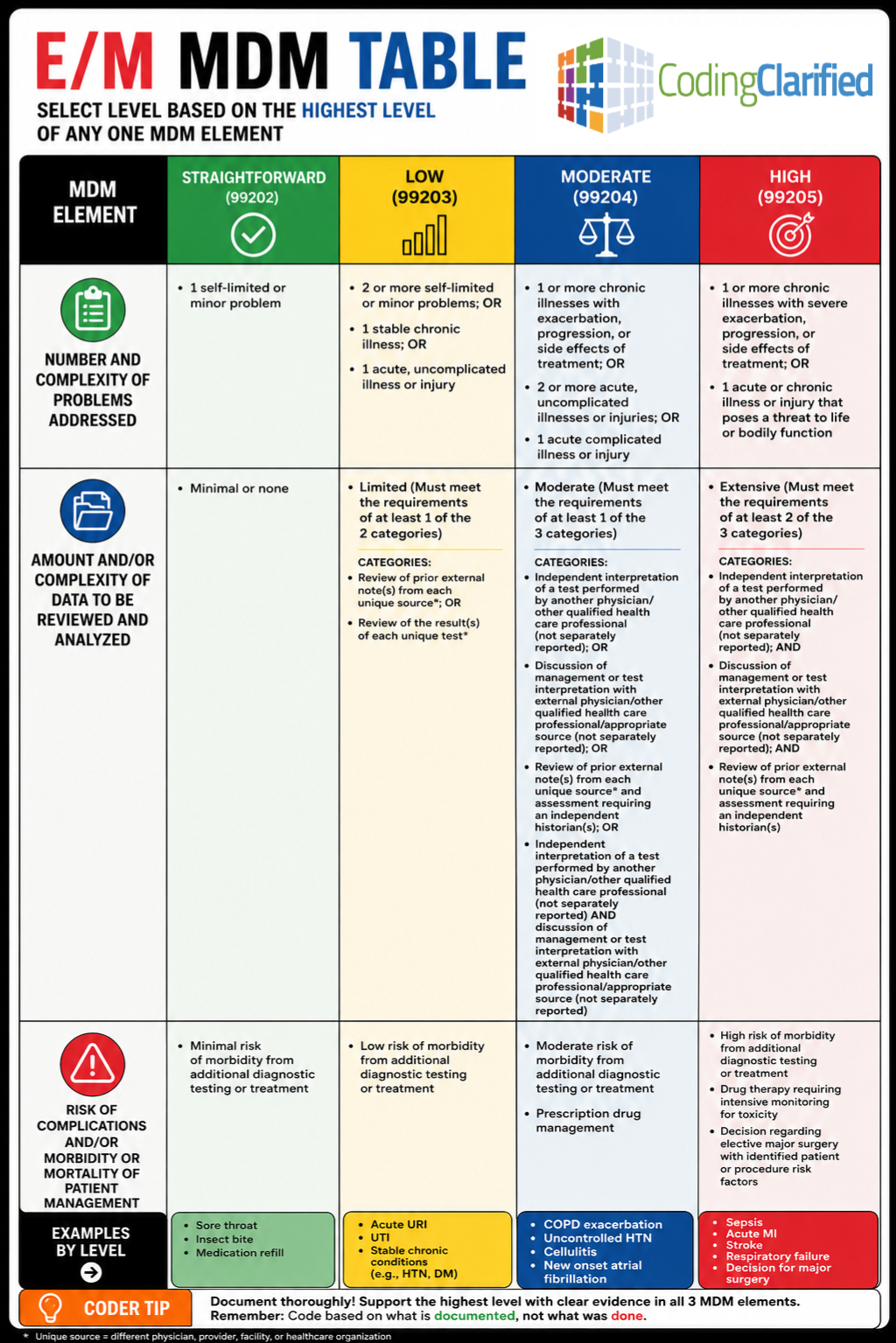
The 2026 E/M MDM Table (Updated Overview)
First and foremost, the Medical Decision Making (MDM) table remains the foundation of E/M coding. However, in 2026, the AMA places greater emphasis on:
- Cognitive Work Recognition
- Data interpretation complexity (including AI-supported data)
- Risk assessment tied to patient management decisions
Key Components of MDM (Still Required)
- Number and complexity of problems addressed
- Amount and/or complexity of data reviewed and analyzed
- Risk of complications and/or morbidity or mortality
What’s New for 2026
- Greater recognition of provider interpretation of AI-generated insights
- Expanded definition of data review, including digital and remote inputs
- Clarification that clinical judgment still overrides automated suggestions
Coding Tip:
Even if AI tools assist in analysis, the provider must document their independent interpretation to support MDM level selection.
New 2026 CPT Codes for Digital Health & AI
Next, one of the most important updates for 2026 involves digital health services and AI-related coding.
Remote Physiologic Monitoring (Updated Focus)
- 99453 – Initial setup and patient education
- 99454 – Device supply with daily recordings
What’s New
- Recognition of short-term monitoring (2–15 days)
- Increased clarity on data collection vs. provider interpretation
Emerging AI-Related Services
Although still evolving, 2026 introduces guidance supporting:
- AI-augmented clinical data review
- Decision-support tools used during patient care
- Documentation of physician oversight when AI is utilized
Important:
AI does not replace provider work—instead, it enhances it. Therefore, coding must reflect the physician’s final decision-making responsibility.
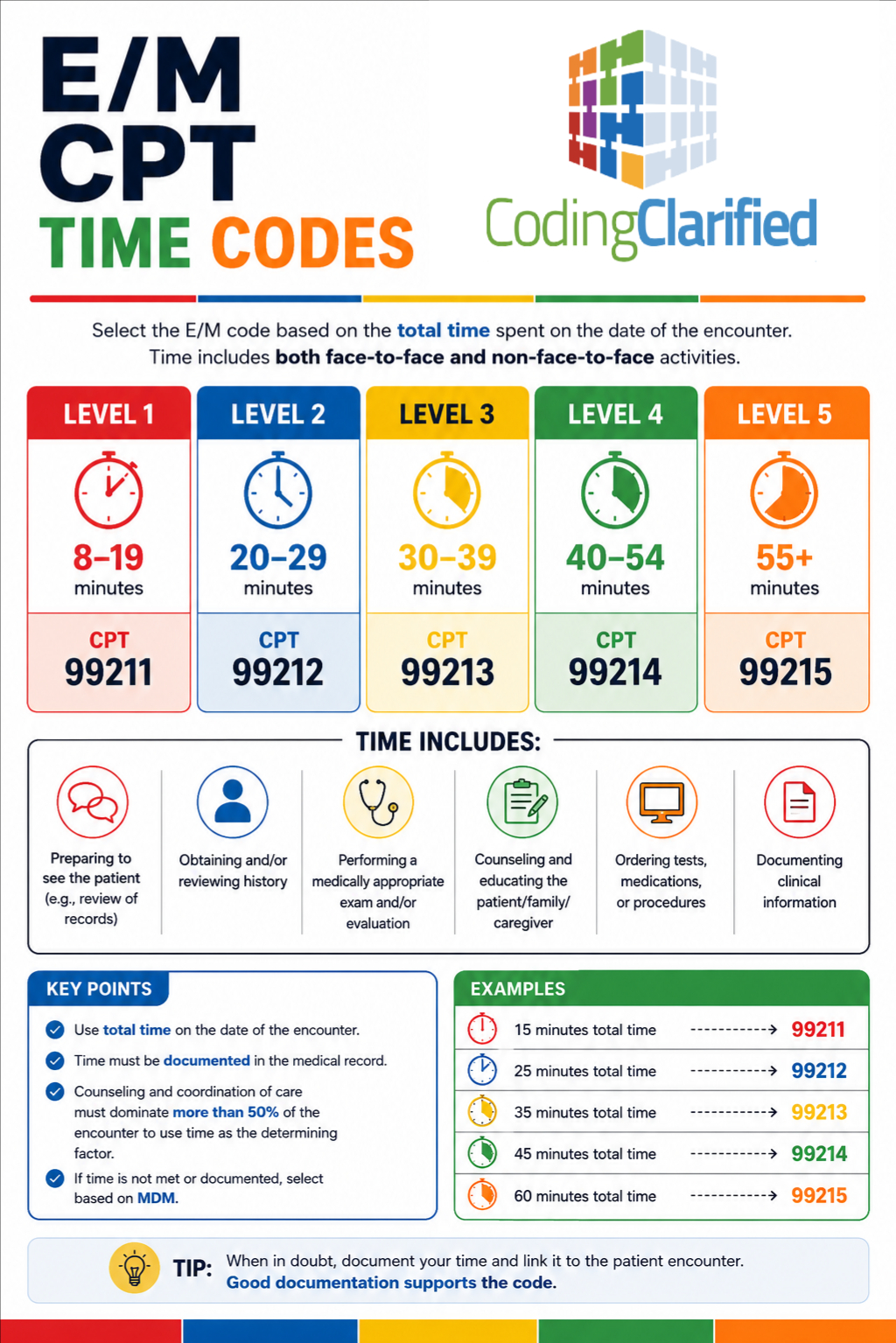
Total Time vs. MDM: 2026 Selection Criteria
In addition to MDM updates, time-based coding has also been refined.
Key Change for 2026
Previously, E/M coding relied on time ranges. However, in 2026, the guidelines shift toward:
Minimum Time Thresholds
This means:
- Providers must meet a specific minimum time to qualify for a code
- Time no longer falls within flexible ranges
When to Use Time vs. MDM
| Use MDM When | Use Time When |
|---|---|
| Complexity drives the visit | Counseling/coordination dominates |
| Multiple conditions or risks | Total time is clearly documented |
| Data review is significant | Minimal complexity but extended time |
Transition Tip:
Because of this change, documentation must clearly state total time spent on the date of the encounter, including non-face-to-face work.
AI-Assisted Coding and Documentation in 2026
Another major shift is the integration of AI-assisted coding tools.
How AI Impacts E/M Coding
- Assists with data aggregation
- Helps identify documentation gaps
- Supports code suggestions
However…
- Providers must validate all AI outputs
- Coders must ensure documentation supports the final code
- Compliance still depends on human clinical judgment
Best Practice:
Always code based on what is documented and medically necessary, not what AI suggests.
Remote Monitoring and Digital Health Expansion
Furthermore, 2026 continues expanding remote care models, including:
- Remote physiologic monitoring (RPM)
- Remote therapeutic monitoring (RTM)
- Short-duration monitoring options
As a result, coders must understand:
- Device requirements
- Data transmission rules
- Provider interaction thresholds
Common 2026 E/M Coding Mistakes to Avoid
Even with clearer guidelines, errors still occur. Therefore, avoid these common pitfalls:
- Relying on AI without provider documentation
- Confusing data review with data interpretation
- Using time without meeting minimum thresholds
- Overlooking risk level documentation
- Failing to support MDM with clear clinical reasoning
How to Stay Compliant in 2026
To remain compliant, coders should:
- Review updated AMA CPT guidance regularly
- Focus on MDM accuracy first
- Ensure documentation reflects clinical thought process
- Understand how AI tools impact—but do not replace—coding rules
- Stay current with payer-specific policies
Coding Clarified Final Thoughts: The Future of E/M Coding
In conclusion, 2026 E/M coding guidelines continue the shift toward smarter, more accurate coding. While AI and digital health tools are becoming more common, the core principle remains the same: documentation must support medical necessity and decision-making.
Ultimately, coders who understand both traditional MDM and modern technology integration will be best prepared for success.
Related Reading
Be sure to read our full guide:
How AI is Changing Medical Coding in 2026