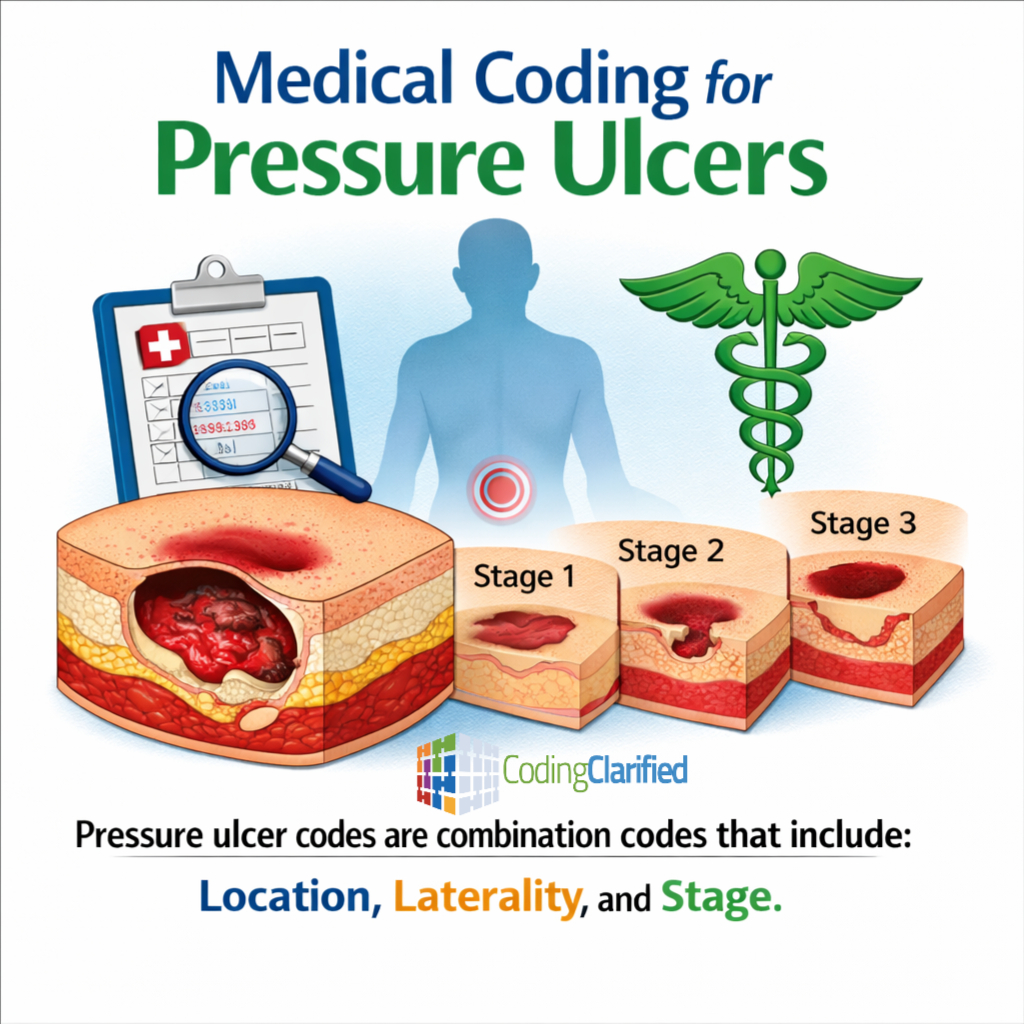
Stages, Guidelines & Coding Tips (ICD-10-CM)
Pressure ulcers (also called pressure injuries or decubitus ulcers) are a high-risk, high-scrutiny diagnosis in medical coding. The accuracy of Medical Coding for Pressure Ulcers impacts quality reporting, reimbursement, HCC risk adjustment, and hospital-acquired condition (HAC) tracking.
For coders, accuracy is critical.
What Is a Pressure Ulcer?
A pressure ulcer is localized damage to the skin and/or underlying tissue, usually over a bony prominence, caused by prolonged pressure or pressure combined with shear.
Common locations:
-
Sacrum
-
Heels
-
Hips
-
Elbows
-
Ankles
-
Occiput (back of head)
ICD-10-CM Category: L89
Pressure Ulcer Codes
Pressure ulcers are coded from Category L89 in ICD-10-CM.
Codes are based on:
-
Anatomical site
-
Laterality
-
Stage
All three components must be documented.
Pressure Ulcer Stages (Clinical & Coding Overview)
Stage 1
-
Non-blanchable erythema
-
Intact skin
Stage 2
-
Partial-thickness skin loss
-
Blister or shallow open ulcer
Stage 3
-
Full-thickness skin loss
-
Subcutaneous fat visible
-
No exposed bone, tendon, or muscle
Stage 4
-
Full-thickness tissue loss
-
Exposed bone, tendon, or muscle
Unstageable
-
Covered by slough or eschar
-
Depth cannot be determined
Deep Tissue Pressure Injury (DTPI)
-
Persistent non-blanchable deep red, maroon, or purple discoloration
ICD-10-CM Official Guidelines Highlights
Code Site + Stage Together
Pressure ulcer codes are combination codes that include:
-
Location
-
Laterality
-
Stage
Example structure:
L89.1__ (Upper back)
L89.6__ (Heel)
If the Stage Is Not Documented
-
Assign the unspecified stage code
-
BUT this often triggers payer scrutiny
Tip: Query when appropriate.
If Ulcer Progresses to a Higher Stage
If a patient is admitted to an inpatient hospital with a pressure ulcer at one stage and it progresses to a higher stage, two separate codes should be assigned: one code for the site and stage of the ulcer on admission and a second code for the same ulcer site and the highest stage reported during the stay
If Healed at Time of Encounter
-
Do NOT code a healed pressure ulcer.
-
If healing but still present, code the documented stage.
Present on Admission (POA)
Hospitals must report POA indicators.
This impacts:
-
Quality metrics
-
Hospital-acquired condition reporting
-
Reimbursement
Coding Tips for Pressure Ulcers
Always Look for:
-
Exact site
-
Laterality (right, left, bilateral)
-
Stage
-
POA status (facility setting)
-
Documentation of infection (if present)
Do Not Confuse:
-
Pressure ulcer
-
Non-pressure chronic ulcer (L97 category)
-
Diabetic ulcer (E08–E13 with L97 combination)
They are coded differently.
Infection with Pressure Ulcer
If provider documents:
-
Pressure ulcer with cellulitis
-
Pressure ulcer with osteomyelitis
Code:
-
L89 code first
-
Additional code for infection
Follow sequencing guidelines based on documentation.
Common Coding Errors
-
Coding both Stage 2 and Stage 3 when the ulcer progressed (only the highest stage)
-
Forgetting laterality
-
Using an unspecified stage when documentation supports specificity
-
Coding healed ulcers
-
Missing deep tissue pressure injury classification
Risk Adjustment & Reimbursement Impact
Stage 3 and Stage 4 pressure ulcers:
-
May affect MS-DRG assignment
-
May qualify as MCC/CC in an inpatient setting
-
Impact quality reporting and penalties
Accurate staging matters.
Real-World Documentation Tips for Coders
Encourage providers to document:
-
Exact location (right heel vs heel)
-
Stage
-
If present on admission
-
If associated with infection
-
If due to the device (medical device-related pressure injury)
Quick Coding Example
Documentation:
“Stage 3 pressure ulcer of the right heel, present on admission.”
Code:
L89.613 – Pressure ulcer of right heel, stage 3
Final Clarified Tip
Pressure ulcer coding is not just about selecting L89.
It requires:
-
Understanding staging
-
Applying ICD-10-CM guidelines
-
Monitoring documentation accuracy
-
Knowing quality reporting implications
When in doubt — query for clarity.
Medical Coding and Casual Relationships
Medical Coding Chronic Kidney Disease
American Academy of Dermatology